Potential Dangers of Rapid Opiate Detox
Rapid opiate detox uses opioid antagonist medications such as naltrexone to displace opioids from the opioid receptors in the brain and central nervous system, essentially blocking and counteracting the opioid effects and precipitating withdrawals.
The potential dangers of rapid opiate detox are well documented and the procedures remain controversial.
About Rapid Opiate Detox
According to the National Collaborating Centre for Mental Health (UK), “The reported advantage of using ultra-rapid or rapid detoxification with anesthesia or sedation is that the duration of withdrawal symptoms is shortened and discomfort is minimized through the anesthesia or sedation.”
On their own, opiate withdrawals are, generally, not considered life threatening, but, the immediate reversal of opioid effects in a rapid opiate detox can be excruciatingly painful and lead to many adverse scenarios and dangerous health risks. Therefore, the antagonist medication is usually provided under sedation or anesthesia in a medically supervised environment where complications during and following the procedure can be immediately attended to.
Clonidine and other medications are used to manage the severity of the ensuing withdrawals and afterwards, the patient is maintained on an antagonist medication to prevent relapse.
Potential Dangers as Found in Randomized Control Tests
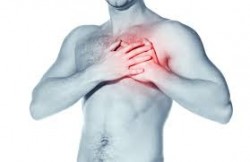
Rapid opiate detox can cause cardiovascular problems.
In randomized control tests, the potential dangers of rapid opiate detox included both complications during the procedure and in the post detox stages including:
- Severe respiratory depression and failure, excessive sedation leading to respiratory depression (requiring intubation), bronchospasms and bradycardia
- Decreased oxygen levels causing hypoxia and other complications including organ damages
- Cardiovascular problems including hypotension, hypertension, irregular heart rate and failure
- Death
- Pneumonia – anaesthesia associated aspiration.
- Delirium, hallucinations, extreme agitation
For people with compromised health issues such as liver disease, pulmonary or cardiovascular problems, diabetes, mental health disorders, or diminished health in any capacity, undergoing anesthesia can be dangerous. In many instances, the patient is bombarded with medications throughout the procedure and immediately thereafter contributing to the potentially dangerous risks.
Post-Detox Dangers
In the post detox phase, some people continue to suffer moderate to severe withdrawals, especially those who have been chronic and long term opiate users and those with co-existing health conditions. In chronic opioid addicts, the post-detox withdrawal severity has led to relapse and the possibility of using higher potency and doses of opioids to overcome the mechanisms or the antagonist medications they return home with, causing overdose.
Cases of suicide and overdose should not be disregarded because the expectancies surrounding this type of treatment may be more than the actual benefits they may receive.


 Pros and Cons of Rapid Detox Programs -
Rapid detox programs, though rather controversial, have both benefits and negative aspects associated with the help that is provided by them. Patients who are addicted to heroin or certain types of prescription painkillers such as Oxycontin or Oxycodone can benefit from rapid detox programs but only if they are aware of the importance of seeking ...
Pros and Cons of Rapid Detox Programs -
Rapid detox programs, though rather controversial, have both benefits and negative aspects associated with the help that is provided by them. Patients who are addicted to heroin or certain types of prescription painkillers such as Oxycontin or Oxycodone can benefit from rapid detox programs but only if they are aware of the importance of seeking ...  What Are Rapid Detox Centers, and How Can They Help? -
Rapid detox is a generally safe and effective way to overcome substance dependency within a relatively short period of time.
What Are Rapid Detox Centers, and How Can They Help? -
Rapid detox is a generally safe and effective way to overcome substance dependency within a relatively short period of time.  How Does Rapid Opiate Detox Work? -
Rapid opiate detox is shortened version of standard detox in which the user is quickly treated for opiate dependence using unconventional methods such as induced coma and intravenous medications. The procedure is performed in an intensive care unit in the hospital or in a hospital like setting in which 24-hour medical monitoring is provided. Here’s ...
How Does Rapid Opiate Detox Work? -
Rapid opiate detox is shortened version of standard detox in which the user is quickly treated for opiate dependence using unconventional methods such as induced coma and intravenous medications. The procedure is performed in an intensive care unit in the hospital or in a hospital like setting in which 24-hour medical monitoring is provided. Here’s ...  How Does Rapid Detox Work? -
There are different types of accelerated detox methods using antagonist medications to precipitate immediate opioid withdrawals with the expectancy of shortening their durations and minimizing their effects. Ultra-rapid detox treatments are commonly performed under heavy sedation or anesthesia with the procedures lasting 5-6 hours while rapid detox treatments use milder sedation methods for the duration ...
How Does Rapid Detox Work? -
There are different types of accelerated detox methods using antagonist medications to precipitate immediate opioid withdrawals with the expectancy of shortening their durations and minimizing their effects. Ultra-rapid detox treatments are commonly performed under heavy sedation or anesthesia with the procedures lasting 5-6 hours while rapid detox treatments use milder sedation methods for the duration ...  5 Benefits of Undergoing Rapid Opioid Detox -
Learn about the benefits of choosing a rapid detox program for your opioid addiction recovery.
5 Benefits of Undergoing Rapid Opioid Detox -
Learn about the benefits of choosing a rapid detox program for your opioid addiction recovery.